Blood transfusions

Blood transfusion is a medical treatment that replaces blood lost through injury, surgery, or disease. The blood enters through a intravenous drip into a patients vein. To avoid a transfusion reaction, donated blood must be compatible with the blood of the patients who is receiving the transfusion. A "cross match" is undertaken to ensure the donor's red blood cells (RBCs) match against the recipient's serum. To perform a cross match, a small quantity of the recipient's serum is mixed with a small amount of the donor RBCs. The mixture is then examined under a microscope. If the given transfusion is incompatible, the donor RBCs are agglutinated by antibodies in the recipient's serum.
Components of the immune system involved in the abnormal response of the body
- Antigens- If the antigens on the red blood cell is complementary to the antibodies of the patient's blood agglutination will occur.
- Antibodies- If the antibody encounters foreign antigens in blood, the antibodies will destroy the foreign blood.
- Red blood cells- Antibodies in the patient's blood will bind to the antigens presented on the foreign red blood cells of the donor causing RBC's to clump; agglutination.
- Antibodies- If the antibody encounters foreign antigens in blood, the antibodies will destroy the foreign blood.
- Red blood cells- Antibodies in the patient's blood will bind to the antigens presented on the foreign red blood cells of the donor causing RBC's to clump; agglutination.
How the normal body functioning is affected
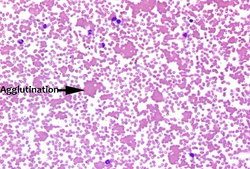
Agglutination is when there is a clump of cells such as bacteria or red blood cells in the presence of an antibody. The antibody binds numerous particles and joins them, creating a large structure. Specifically, haemagglutination is the clumping of red blood cells and this occurs when people are transfused with the wrong blood type.
When the incompatible blood type enters the patients body, the body registers it as a foreign substance, as the antigen blood types are not the same.
The sequence of steps followed by the incorrect match of blood types:
1. The foreign substance is engulfed by a macrophage which combines an antigenic fragment with its own class II MHC marker (Major Histocompatibility Complex).
2. The antigen/ MHC complex is displayed on the surface of the macrophage.
3. The macrophage presents the antigen to a T helper cell.
4. The T helper cell presents the antigen to an immature B cell.
5. The B cell divides producing many B plasma cells which secrete specific antibodies (which act against the foreign substance) and a few B memory cells which remain in the lymphatic system.
Some antibodies may activate the complement cascade, a series of enzyme-catalysed reactions involving protein fragments.The cascade finishes with the formation of a "membrane attack complex", a large molecule that pierces a hole in the cell membrane of the blood cell. Other antibodies bind to the donor RBCs and cause them to agglutinate. The agglutinated cells may survive or may be removed from the circulation by the macrophages.
Macrophages discard the antibody-coated cells from circulation through the process of phagocytosis. Macrophages have receptors that bind to the antibodies and another receptor that joins to complement fragments. The incompatible RBC's are rapidly destroyed after antibody binding.
In addition, this antibody response may cause crucial hemolytic transfusion reactions.
The sequence of steps followed by the incorrect match of blood types:
1. The foreign substance is engulfed by a macrophage which combines an antigenic fragment with its own class II MHC marker (Major Histocompatibility Complex).
2. The antigen/ MHC complex is displayed on the surface of the macrophage.
3. The macrophage presents the antigen to a T helper cell.
4. The T helper cell presents the antigen to an immature B cell.
5. The B cell divides producing many B plasma cells which secrete specific antibodies (which act against the foreign substance) and a few B memory cells which remain in the lymphatic system.
Some antibodies may activate the complement cascade, a series of enzyme-catalysed reactions involving protein fragments.The cascade finishes with the formation of a "membrane attack complex", a large molecule that pierces a hole in the cell membrane of the blood cell. Other antibodies bind to the donor RBCs and cause them to agglutinate. The agglutinated cells may survive or may be removed from the circulation by the macrophages.
Macrophages discard the antibody-coated cells from circulation through the process of phagocytosis. Macrophages have receptors that bind to the antibodies and another receptor that joins to complement fragments. The incompatible RBC's are rapidly destroyed after antibody binding.
In addition, this antibody response may cause crucial hemolytic transfusion reactions.
If the wrong blood type is transfused hemolytic transfusion reaction can occur.
Acute Hemolytic Transfusion Reaction symptoms:
- Shock
- Anxiety
- Fever
- Chills
- Fainting or breathing problems
- Pain in your abdomen, chest, or back
- Kidney Failure - if serious can lead to death
Delayed Hemolytic Transfusion Reaction symptoms:
- A high fever and chills
- Blood in urine
- Dizziness or fainting
- Headaches
- Jaundice
Prevention / Treatment
Although cross matching should prevent incompatible ABO blood group antigens from triggering this type of reaction, however human error sometimes leads to the "wrong blood" being given during a transfusion.
If agglutination and symptoms start to occur, the transfusion must be immediately stopped and these should be considered;
If agglutination and symptoms start to occur, the transfusion must be immediately stopped and these should be considered;
- Keep the intravenous (IV) line open with saline.
- Give oxygen and fluid support.
- Control blood pressure and maintain an open airway


